Yes, constipation is a very common cause of rectal bleeding. Seeing blood on your toilet paper or in the bowl is definitely alarming, but it’s often just a sign that you’re straining to pass hard, dry stools. This mechanical stress can cause minor injuries to the sensitive tissue in your anal canal.
The Direct Link Between Constipation And Rectal Bleeding
Think of the delicate lining of your anal canal like a soft, fine fabric. When it's forced to stretch beyond its limit by a large, hard stool, it can easily tear. That’s the simple, direct answer to the question, "does constipation cause rectal bleeding?" The immense pressure from straining during a bowel movement is what triggers the bleeding.
This isn't just a hunch; it's a fact backed by solid medical research. One major study found that people with chronic constipation are over three times more likely to experience rectal bleeding compared to those who aren't constipated. In fact, it was identified as the single strongest risk factor.
All that pushing puts tremendous pressure on the lower rectum and anus. This pressure usually leads to one of two main issues, which are responsible for most cases of bright red rectal bleeding:
Hemorrhoids: These are just swollen veins in your anus and lower rectum. They become inflamed and fragile from all the straining, making them prone to bleeding.
Anal Fissures: Think of these as small, painful paper cuts in the lining of your anal canal. They’re caused directly by the passage of hard, lumpy stool.
Basically, the harder you push, the more likely you are to damage these delicate structures. The good news is that the bleeding is typically bright red, which tells your provider it’s coming from a source low in your digestive tract, like the anus. You can learn more about what it means when you see blood when you wipe in our detailed guide.
Understanding this connection is the first step toward getting relief. By tackling the root cause—constipation—we can often resolve the bleeding and stop it from coming back.
How Hemorrhoids Cause Bleeding When You're Constipated
If you're constipated and see blood, the most likely culprit is hemorrhoids. It's a jarring sight, but it helps to know what's going on. Hemorrhoids aren't some strange growth—they’re just swollen veins in your anus and lower rectum that everyone has. They only become a problem when they get irritated and inflamed.
When you're straining on the toilet, you’re putting a huge amount of pressure on your lower body. That pressure causes the delicate veins down there to swell up. Think of them like little balloons: if you keep forcing air into them, the walls get thin and fragile, ready to leak with the slightest friction.
That’s exactly what happens when a hard, dry stool scrapes past these over-inflated, sensitive veins. The friction is enough to tear the surface and cause them to bleed.
Bleeding from hemorrhoids has a few tell-tale signs. Seeing them can give you a clue about what's happening, but remember, only a healthcare provider can give you a definite diagnosis.
Here’s what you might notice:
Bright Red Blood: The blood is almost always bright red. That’s because it’s fresh, coming from a source right near the exit, so it hasn’t had time to darken.
Painless Bleeding: Often, the bleeding itself doesn't hurt, even if the hemorrhoids are causing other issues like itching or discomfort.
Blood on Toilet Paper or in the Bowl: You’ll probably spot streaks of blood on the toilet paper after you wipe, or see a few drops floating in the toilet water.
This is an incredibly common issue. In the United States, about 1 in 20 people deal with symptomatic hemorrhoids. If you want to go deeper on this, you can explore why hemorrhoids are so common in our other article.
Hemorrhoids are the most frequent cause of rectal bleeding. Their rich blood supply makes them prone to bleeding when irritated by hard stools and straining, which is why managing constipation is a key part of treatment. Find out more about the connection between constipation and blood in stool on Medical News Today.
The link is crystal clear. The strain from being constipated inflames hemorrhoids, and the passage of hard stool makes them bleed. This is why the best long-term strategy is to get your bowel habits sorted out. By softening your stool and not having to strain, you give those swollen veins a chance to heal and stop future bleeding before it starts.
Anal Fissures: The Other Reason Constipation Causes Bleeding
Hemorrhoids get all the attention, but they aren't the only cause of bleeding when you're constipated. Meet the other common culprit: the anal fissure.
Think of a paper cut on your finger—that same kind of sharp, painful little tear can happen in the delicate lining of your anal canal. That’s an anal fissure. It’s most often caused by the trauma of passing a large, hard stool. The rigid stool essentially scrapes against the sensitive tissue and tears it on the way out.
This is why, unlike some hemorrhoid bleeding, a fissure almost always comes with a sharp, severe pain. You’ll feel it during the bowel movement and sometimes for hours afterward. The bleeding is typically bright red but usually less than you’d see with a hemorrhoid—often just a few streaks on the toilet paper or a drip in the bowl.
Anal fissures are notorious for creating a frustrating cycle that can make constipation even worse. The intense pain from a bowel movement can create a very real, subconscious fear of going to the bathroom. You might find yourself clenching your sphincter muscles and holding it in just to avoid the pain.
But this avoidance is counterproductive. Holding it in only gives stool more time to become harder and drier in your colon. The next bowel movement is then even more painful, which can easily re-tear the fissure or stop it from healing altogether.
It’s a vicious loop:
Constipation causes hard stools.
Passing a hard stool creates a painful anal fissure.
The fear of pain makes you avoid going to the bathroom.
Holding it in makes constipation worse, and the cycle starts again.
This is why medical authorities like the Mayo Clinic point to chronic constipation as one of the top causes of anal fissures. The strain and friction from passing hard stools are the perfect recipe for tearing the anal lining, leading to that signature sharp pain and bright red blood. If you're looking for more information on the healing process, it's helpful in understanding the stages of fissure healing.
Breaking this cycle requires a two-pronged attack: softening your stool to prevent more trauma and using targeted treatments to help the fissure heal. This is where specialized topical creams, like those with the prescription ingredient nifedipine, can be a game-changer. They work by relaxing the anal sphincter muscle, which improves blood flow to the tear and gives it a chance to heal properly. You can learn more about how nifedipine helps heal anal fissures right here in our guide.
What The Color And Amount Of Blood Reveals
Seeing blood after you poop is instantly alarming. But before you panic, take a breath. The color and amount of blood you see can tell you a lot about what's going on and how quickly you need to act.
Most of the time, seeing bright red blood on the toilet paper or a few drops in the toilet bowl means the bleeding is happening close to the exit—in your lower rectum or anus. This is the classic sign of bleeding caused by constipation, usually pointing to either hemorrhoids or an anal fissure. While you definitely need to address it, it's generally not a five-alarm fire.
This quick guide breaks down the two most common culprits behind that bright red blood.
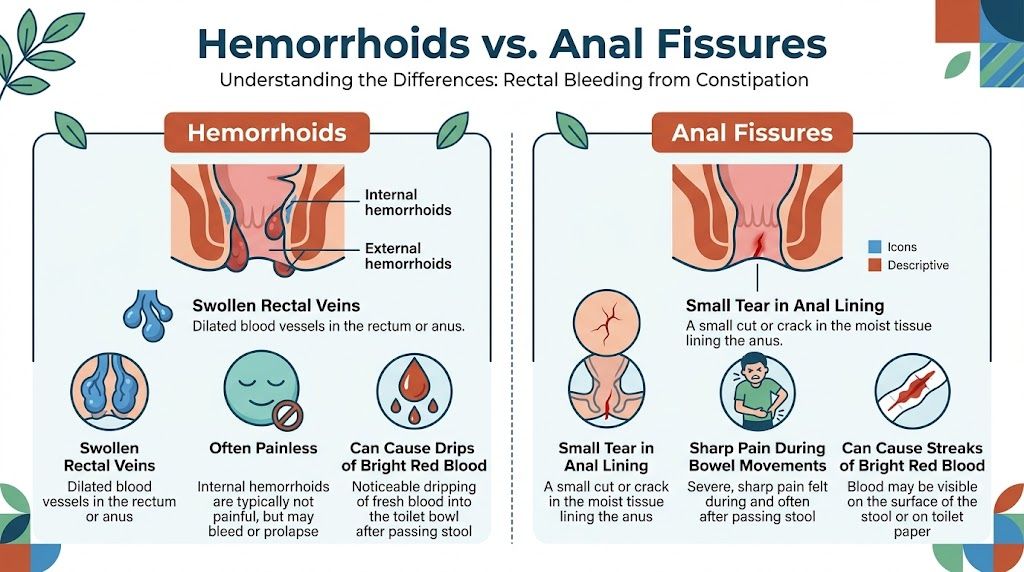
As you can see, both can cause bright red bleeding. The big difference-maker is often pain. Fissures usually hurt—a lot—while hemorrhoids are often painless.
The chart below breaks down what different symptoms could mean and when it’s time to get a professional opinion.
| Symptom | Common Causes | Recommended Action |
|---|---|---|
| Bright red blood on toilet paper or in the bowl | Hemorrhoids, anal fissures | Address constipation, use at-home care, and take the Bummed quiz. |
| Dark red or maroon blood mixed with stool | Bleeding higher up in the colon | Schedule an appointment with your provider or a specialist promptly. |
| Black, tar-like stool | Bleeding in the stomach or upper small intestine | This is a more urgent sign. Contact your provider right away. |
| Heavy, continuous bleeding or passing clots | Could be a more severe tear or other serious condition | Seek immediate medical care at an urgent care or ER. |
Knowing these differences helps you move from "freaking out" to "figuring it out."
While a little bright red blood is common, some signs are non-negotiable red flags that demand immediate medical attention. The color of the blood changes the longer it’s been in your digestive tract, which helps pinpoint where the problem is.
According to experts at the Cleveland Clinic, dark red, maroon, or black, tar-like stools are a sign that bleeding is happening much higher up in your gut, like in your colon or stomach. This is far more serious and should never be ignored.
Any rectal bleeding is worth discussing with a provider, but some symptoms are true emergencies. If you have heavy bleeding, feel dizzy or faint, or have severe abdominal pain, it’s time to head to the ER.
Listen to your body. Here are the symptoms that mean you should call your provider immediately or go to the nearest emergency room:
Heavy or continuous bleeding that won’t stop
Passing large clots of blood
Feeling dizzy, lightheaded, or like you might faint
Severe pain in your abdomen or rectum
A rapid heartbeat, chest pain, or shortness of breath
Recognizing these signs helps you know when to seek help right away versus when you can schedule a regular (or telehealth) appointment.
How To Stop The Bleeding And Get Relief At Home

Let's get straight to it: the best way to stop the bleeding is to tackle the constipation that’s causing it. By making a few key changes at home, you can soften your stool, stop the straining, and finally give your body a chance to heal.
This isn’t about a total life overhaul. It’s about small, consistent adjustments to your diet, hydration, and bathroom habits that make a huge difference.
Think of dietary fiber as your digestive system’s best friend. It’s essential for creating softer, bulkier stools that are much easier to pass. Fiber works by soaking up water, which adds weight and volume to your poop, helping it move along smoothly without a fight.
You can easily up your fiber game with foods like these:
Fruits: Pears, berries, and apples (keep the skin on!) are fantastic. And yes, prunes and prune juice are famous for a reason—they really work.
Vegetables: Load up on broccoli, carrots, and Brussels sprouts.
Whole Grains: Ditch the white bread and pasta for whole-wheat versions. Oats and quinoa are your friends, too.
Legumes: Beans, chickpeas, and lentils are true fiber powerhouses.
But remember, fiber can't work its magic alone. It needs water. Without enough fluids, fiber can actually make constipation worse. So, aim to drink plenty of water throughout the day. For more ideas, check out our complete guide on high-fiber foods for constipation.
Believe it or not, how you go is just as important as what you eat. Straining on the toilet puts a ton of pressure on the veins and delicate tissues around your anus. This is what directly leads to the bleeding from hemorrhoids and fissures we've been talking about.
Here are a few simple tips for better bathroom ergonomics:
Use a Footstool: Propping your feet up on a small stool changes your body’s posture to something closer to a natural squat. This straightens out your colon, making it way easier for stool to pass without straining.
Don't Linger: Stop scrolling on your phone! Sitting on the toilet for long stretches encourages subconscious straining and puts extra pressure on your rectum.
Listen to Your Body: When you feel the urge to go, go. Holding it in allows more water to get absorbed from your stool, making it harder, drier, and more difficult to pass later.
According to Franciscan Health, gentle movement is another powerful tool. Once your provider gives the okay, even short walks can help stimulate your intestines and promote regular bowel movements.
If you want to dive deeper into managing and preventing constipation, you can find a helpful guide on natural remedies for constipation. Combining these simple lifestyle changes is a powerful way to find relief from both constipation and the bleeding it causes.
When You Should See A Provider About Rectal Bleeding
Most of the time, a little bleeding from constipation can be handled at home. An occasional speck of bright red blood on the toilet paper is common and isn't usually a reason to panic. But it's also not something you should ever ignore, especially if it becomes a regular thing or comes with other worrying symptoms.
Getting a real diagnosis is the most important step. Even if you're pretty sure it's just hemorrhoids or a fissure, having a provider confirm it is smart. It rules out anything more serious and makes sure you’re on the right track for treatment. The experts at the Mayo Clinic agree: you should see a provider if at-home care doesn't help or if you’re concerned about your symptoms.
It’s time to make an appointment if your rectal bleeding checks any of these boxes:
It continues for more than a week. A single episode of spotting is one thing. Bleeding that sticks around for days or keeps coming and going needs to be looked at.
It’s accompanied by other concerning symptoms. Pay attention if the bleeding comes with major pain, a change in your bowel habits (like new constipation or diarrhea), or you're losing weight without trying.
The amount of blood is increasing. If you’re starting to see more blood than you did before, it’s a sign the issue might be getting worse.
Don't let embarrassment stop you from getting answers. Rectal bleeding is incredibly common, and getting a proper diagnosis is the first step toward feeling better.
Thankfully, modern telehealth makes getting an expert opinion easier and more private than ever. Services like Bummed let you get a fast, discreet medical review from a board-certified provider without even leaving your house. After a quick online intake form, a provider can often give you a same-day diagnosis and, if it’s right for you, send a personalized prescription cream straight to your door. It’s a direct path to effective, science-backed treatment without the hassle of an in-person visit.
If you're dealing with persistent rectal bleeding, pain, or other uncomfortable symptoms, don't wait for relief. With Bummed, you can get a same-day diagnosis and a personalized prescription treatment plan from a board-certified provider, all from the comfort of home. Start your confidential online visit with Bummed today and get on the path to feeling better.
Frequently Asked Questions About Constipation and Rectal Bleeding
How long does bleeding from constipation normally last?
Bleeding from constipation—whether it's from a hemorrhoid or a small tear like an anal fissure—is usually very short-lived. You might just see a small amount of bright red blood during that one trip to the bathroom. At most, it might hang around for a day or two if the area gets irritated again. The real red flag is persistence. If you're seeing blood with every single bowel movement, or if the bleeding drags on for more than a few days, that’s your body’s signal to talk to a provider. Continuous bleeding needs a proper look to rule out other issues and get you on the right treatment plan.
Can certain foods worsen both constipation and bleeding?
Absolutely. Some foods are notorious for causing constipation, which is the first domino to fall. Diets that are low in fiber but high in processed stuff—think fast food, lots of cheese, and pre-packaged snacks—are the usual suspects. They can lead to hard, dry stools that are a real struggle to pass. By making your stool harder, these foods indirectly dial up the odds of getting a painful fissure or flaring up a hemorrhoid. The counter-move is simple: focus on a diet loaded with fruits, vegetables, and whole grains. And just as important, drink plenty of water to help all that good fiber do its job.
Is it safe to use over-the-counter creams for bleeding?
While some over-the-counter (OTC) products might give you a bit of temporary relief from itching or mild pain, they often don’t fix the real problem. Most OTC creams simply aren’t designed to heal something like an anal fissure, which needs specific ingredients to help relax the muscle and boost blood flow to the area. For stubborn or painful symptoms, a prescription-strength, compounded medication is often the answer. It’s formulated to deliver more targeted and effective treatment by combining multiple evidence-based ingredients in one cream.
Bummed content is for general education and should never replace professional medical advice that considers your individual health. If you think you’re experiencing a medical emergency, call 911 or head to the nearest emergency department.
Prescription products require an online consultation with a physician who will determine if a prescription is appropriate.
