Shifting in your chair, avoiding the toilet, or wondering why a tiny area can cause such outsized misery? Anal pain, itching, burning, and swelling can make ordinary things feel difficult. Sitting at work hurts. Walking feels irritating. Bowel movements become something you dread.
For many people, lidocaine hydrocortisone cream is one of the first prescription treatments that comes up. It is commonly used to calm symptoms from hemorrhoids, anal fissures, and related irritation. It can help quickly, especially when the goal is to reduce pain and itching fast. But in practice, symptom relief and actual healing are not always the same thing. That distinction matters.
Understanding Anorectal Discomfort and Initial Relief
When patients describe hemorrhoids or a fissure, the words are usually simple and direct. “It burns.” “Itches all day.” “It feels sharp.” “I’m afraid to have a bowel movement.” Those symptoms are common, and they deserve treatment, not embarrassment.

Lidocaine hydrocortisone cream is a prescription topical used for anorectal conditions, and these problems affect an estimated 50% of adults in the U.S. by age 50. Standard dosing is a thin film applied 2 to 3 times daily, according to Mayo Clinic guidance on lidocaine and hydrocortisone rectal use.
Why this cream is often the first step
This combination makes sense as an opening treatment because it goes after the symptoms people feel most intensely.
-
Pain and burning: Lidocaine helps numb the area.
-
Itching and swelling: Hydrocortisone helps calm inflamed tissue.
-
Short-term flare control: It can make daily life more manageable while the tissue settles down.
That is useful. It is not trivial relief. If someone has been miserable for days, symptom control matters.
Where patients get stuck
The challenge is that anorectal problems are not all the same. A thrombosed hemorrhoid, an irritated internal hemorrhoid, and a chronic fissure may all hurt, but they do not behave the same way. A cream that quiets symptoms may not fully address the reason symptoms keep returning.
Practical point: If a cream helps for a few hours but your pain keeps coming back after each bowel movement, that often means the underlying problem needs a more specific plan.
Gentle skin care also matters more than many people realize. Overwashing, fragranced wipes, and harsh soaps can keep the area irritated. Some patients benefit from reviewing general principles of managing sensitive skin discomfort, then applying those habits to the perianal area in a cautious, simplified way.
If you want a broader overview of common causes and symptom patterns, this guide on https://bummed.co/the-bummed-guide-to-hemorrhoids-anal-fissures-anal-itching/ is a useful place to start.
How Lidocaine Hydrocortisone Cream Fights Pain and Itching
A good way to understand this cream is to think of it as a two-person team. One ingredient blocks the alarm signal. The other cools down the fire.
Lidocaine blocks the pain message
Lidocaine is the numbing part. It acts as a local anesthetic by inhibiting sodium influx into nerve cells, preventing pain signals from initiating and traveling. Its chemical properties, including a pKa of 7.7, enable it to act rapidly, making it effective for acute anorectal pain, as described in the DailyMed labeling for lidocaine hydrochloride and hydrocortisone acetate cream.
If you want a simple analogy, lidocaine acts like a roadblock on a nerve pathway. The pain signal tries to travel, but it cannot proceed normally.
This is why relief is often noticed shortly after application. While the tissue itself may not be healed, the signal from the irritated nerve endings is reduced.
For longer-term relief, bupivacaine is a more effective solution. Bummed’s prescription treatments include bupivacaine, whereas other over-the-counter options do not. For additional details, refer to this article.
Hydrocortisone cools the inflammatory flare
Hydrocortisone is the anti-inflammatory part. It is a mild corticosteroid. In practical terms, it helps reduce redness, swelling, and itch.
We often describe it as a firefighter. When the skin and lining around the anus are inflamed, they become reactive. They itch more. They swell more. They sting more. Hydrocortisone helps settle that response.
What the combination does well and what it does not
Used together, the ingredients can be very helpful for short-term symptom control.
| What it helps with | Why it helps |
|---|---|
| Sharp pain | Lidocaine numbs irritated nerve endings |
| Itching | Hydrocortisone calms inflamed tissue |
| Burning | Both ingredients can reduce the sensation burden |
| Tenderness during a flare | Temporary local symptom relief |
The important trade-off is this: Relief is not always equivalent to repair. If the underlying issue is ongoing sphincter spasm, persistent constipation, repeated straining, or a deeper fissure, the cream may enhance comfort without fully addressing the cycle.
Key takeaway: Lidocaine hydrocortisone cream serves primarily as a symptom-relief tool. For some patients, this may suffice. For others, it is merely part of a comprehensive treatment plan. Bummed’s prescription creams, however, include ingredients such as nitroglycerin and diltiazem, which can help address the root causes. More information on these ingredients can be found at Bummed’s diltiazem resource and Bummed’s nitroglycerin resource.
Correctly Using Your Lidocaine Hydrocortisone Cream
Technique matters. A good prescription can underperform if it is used inconsistently, applied to unclean skin, or stopped and started in a haphazard way.

How to apply it
For most adults, the usual approach is a thin film applied 2 to 3 times daily. If the prescription includes rectal use, product guidance commonly advises gentle insertion of the applicator a short distance int
Bummed packages all include finger cots for a cleaner application to the anus after cleansing.
A practical routine looks like this:
-
Clean the area gently. Use water or a soft, non-irritating cleanser. Pat dry. Do not scrub.
-
Apply a thin layer externally if the symptoms are on the outside.
-
If your clinician has instructed internal use, consider using finger cots gently.
-
Wash your hands after application.
-
Stick to the prescribed schedule. Random use usually works poorly.
Where patients often go wrong
The most common mistakes are simple.
-
Using too much: More cream does not mean faster healing.
-
Applying to wet or irritated skin after aggressive wiping: This can increase stinging.
-
Skipping bowel habit treatment: If stool remains hard or straining continues, symptoms often persist.
-
Using it longer than intended without reassessment: Steroid-containing creams are usually not meant to become a long-term autopilot solution.
External symptoms versus internal symptoms
External irritation, perianal itching, and thrombosed external hemorrhoid discomfort usually respond best when the cream is placed exactly where the pain is. Internal hemorrhoid irritation may require more careful internal application if your prescription allows for that.
For patients who struggle with placement, this practical guide to https://bummed.co/how-to-put-hemorrhoid-cream-exactly-where-you-need-it-no-fancy-applicator-required/ can help.
Tip: Apply after a bowel movement when possible. That usually keeps the medication in place longer and reduces the urge to wipe it away.
When to pause and ask for help
Contact your provider if the area becomes more irritated, the pain rapidly worsens, or symptoms are not improving. The cream should make things feel calmer, not more inflamed.
Safety Warnings and Side Effects You Should Know
Most patients tolerate lidocaine hydrocortisone cream reasonably well, but “topical” does not mean “use without limits.” The anorectal area absorbs medication differently than intact skin elsewhere, and the wrong use pattern can create new problems.
Common short-term issues
Mild side effects can include temporary burning, stinging, or irritation right after application. Sometimes that is just because the skin is already raw.
A few cautions matter more:
-
Do not use it on autopilot for weeks unless a provider tells you to.
-
Avoid it if you have certain infections or hypersensitivity, because steroid-containing products can worsen some infectious skin conditions.
Pregnancy and postpartum use
Pregnancy and the postpartum period are when anorectal symptoms often surge. Hemorrhoids affect many pregnancies, but safety data on lidocaine hydrocortisone cream during pregnancy and breastfeeding is limited. Cleveland Clinic advises patients to tell their provider if they are pregnant, trying to become pregnant, or breastfeeding, which is why individual review matters so much. See the Cleveland Clinic medication guidance for lidocaine and hydrocortisone skin cream or lotion.
Limited data does not indicate that the medication is consistently unsafe; rather, it suggests that decisions should be individualized. Postpartum tissue changes, active bleeding, tears, and breastfeeding concerns can all influence what is appropriate. In our intake forms, Bummed will inquire if you’re pregnant before deciding on the suitable treatment for you.
GLP-1 medications and constipation-related flare-ups
Another pattern we see more often is anorectal pain in people taking GLP-1 medications. These medicines can slow the gut and contribute to constipation in some patients. When stool gets harder or bowel movements become less frequent, hemorrhoids and fissures often flare.
The important clinical point is not just to numb the area. It is to address the bowel pattern that is feeding the irritation.
Why long-term use is not a great plan
Hydrocortisone can calm inflammation, but prolonged steroid use on delicate skin can raise concerns about skin thinning, irritation, and rebound symptoms when people keep restarting it every time they flare. Lidocaine can also mask pain without fixing the reason the tissue is injured.
Situations that deserve a provider review
-
Persistent bleeding: Especially if the amount increases or the diagnosis is uncertain.
-
Severe pain that feels out of proportion: This can signal something more than a simple hemorrhoid flare.
-
No improvement with short-term treatment: Recurrent symptoms often need a different strategy.
-
Black stools or systemic symptoms: These need prompt in-person evaluation.
Safety rule: If symptoms are escalating, not improving, or no longer fit the label of “just hemorrhoids,” stop guessing and get examined.
Why Compounded Creams Offer Superior Relief
A standard two-ingredient cream can be useful, but it often treats the surface of the problem rather than the full mechanism behind it. That becomes obvious with chronic fissures, mixed hemorrhoid pain, or the patient whose symptoms improve for a few hours and then rebound after every bowel movement.
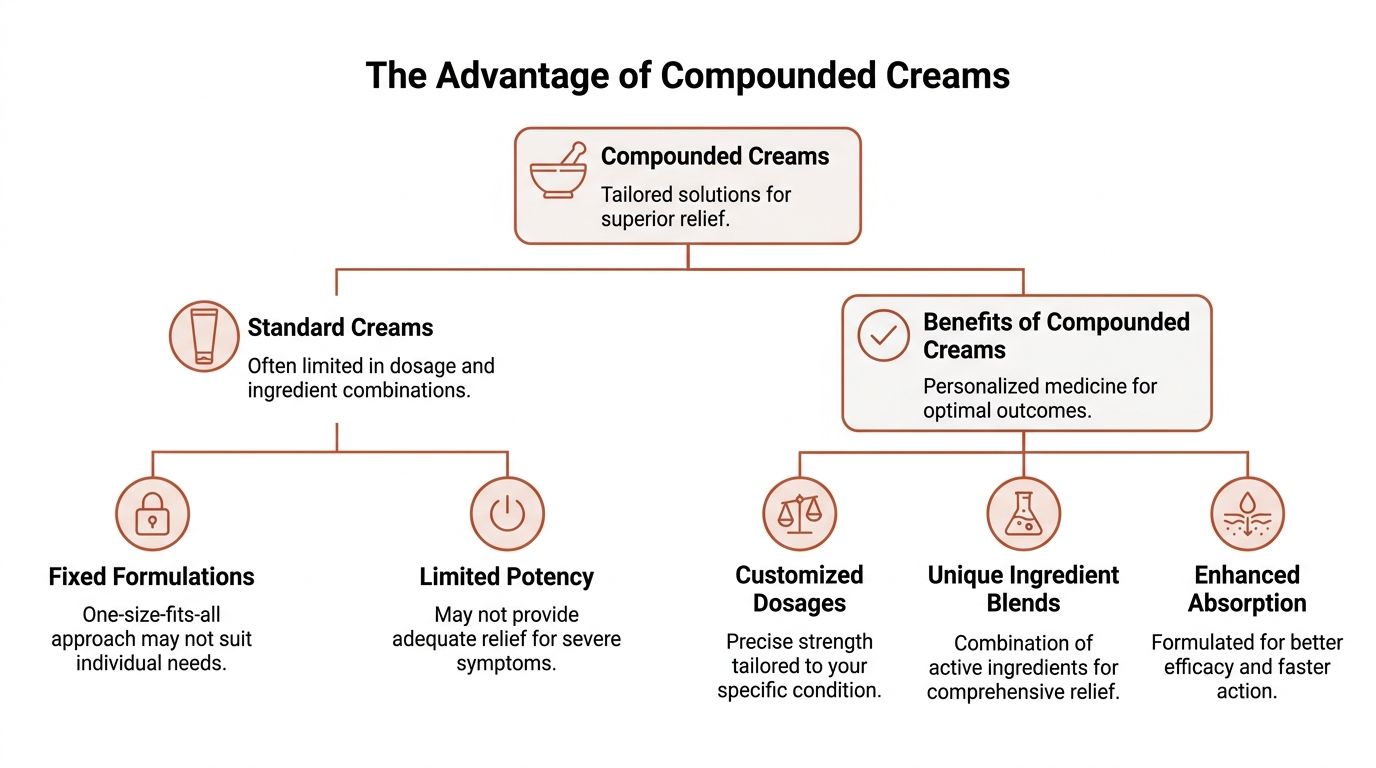
Why two ingredients can fall short
Lidocaine can numb. Hydrocortisone can calm inflammation. But neither directly relaxes a tight internal anal sphincter.
That matters because many painful fissures and some hemorrhoid flares are driven by spasm and pressure. If the muscle stays tight, blood flow can stay poor, bowel movements stay painful, and healing can stall even when the area feels numb for a while.
This is the main limitation of standard lidocaine hydrocortisone cream. It can make symptoms more tolerable without fully interrupting the cycle.
What added ingredients are designed to do
As a colorectal surgeon, Dr. Carmen Fong built compounded anorectal formulas recognizing that many patients have overlapping issues, not one neat diagnosis. These prescriptions may combine lidocaine and hydrocortisone with other active ingredients, which is what makes multi-ingredient formulations distinct.
Here is the clinical logic behind the added agents.
Nitroglycerin
Topical nitroglycerin is used when rapid sphincter relaxation is needed. The idea is straightforward. Relax the internal sphincter, improve local blood flow, and give injured tissue a better chance to heal.
In practice, the trade-off is recognized. Some patients experience headaches and are unable to tolerate it. Nitroglycerin is an ingredient in Bummed’s Rapid Relief cream, which can be found here.
Diltiazem
Topical diltiazem, available in Bummed’s Long-Acting cream, is frequently selected to achieve sustained sphincter relaxation while minimizing systemic side effects compared to nitrates. In practical anorectal care, it serves as a useful choice for addressing recurrent fissure-related pain or for patients who have difficulty tolerating nitroglycerin.
Nifedipine
Topical nifedipine, found in Bummed’s Sensitive Care Rx, is a calcium channel blocker that helps lower internal sphincter tone. It is often considered effective and well-tolerated, particularly in cases where fissure-related pain is prominent.
Metronidazole
Topical metronidazole is not generally the first choice for every patient, but it can be beneficial for particularly inflamed areas or when managing postoperative discomfort. It is selectively included rather than used automatically. Metronidazole is available in both Long-Acting and Rapid Relief creams.
Clinical reality: The best anorectal cream is not always the strongest numbing cream. It is the one that matches the mechanism causing the pain.
Why compounding can be more practical
Compounding allows a clinician to combine medications in ways that reflect the actual diagnosis. That matters when someone has a fissure plus hemorrhoidal swelling, or itching plus spasm, or inflammatory pain plus difficult bowel habits.
A multi-ingredient plan can help by:
-
Targeting more than one driver: Pain, inflammation, spasm, and tissue irritation may all be contributing.
-
Simplifying the routine: One prescription can be easier to follow than several separate products.
-
Reducing trial-and-error: Patients do not have to bounce between partial solutions.
The ingredient ratios used in these formulations were chosen by Dr. Carmen Fong based on years of clinical experience using these medications in practice. That point matters. In anorectal care, small formulation choices can change tolerability and adherence.
If you want background on why some customized prescriptions come from compounding pharmacies rather than standard retail manufacturing, this explainer on https://bummed.co/what-exactly-is-a-compounding-pharmacy-and-why-arent-its-meds-fda-approved/ gives a useful overview.
Getting a Prescription and Accessing Specialized Care
Some patients get lidocaine hydrocortisone cream through a primary care office, urgent care, OB-GYN, dermatologist, or colorectal surgeon. That is a reasonable path, especially when the diagnosis is straightforward and the symptoms are mild.

Traditional visit versus telehealth
An in-person visit has obvious strengths. A clinician can examine the area, confirm whether the problem is a fissure, thrombosed hemorrhoid, dermatitis, abscess, or something else, and prescribe accordingly.
Telehealth can also be very helpful when symptoms fit a common anorectal pattern and the patient wants fast, private access to care. The model is simple. You complete an intake, a licensed clinician reviews the history, and treatment is prescribed if appropriate. For many adults, that means less delay and less embarrassment.
For a broader look at that care model, this article on https://bummed.co/7-ways-telehealth-is-changing-acute-care-for-good/ explains where telehealth fits and where it does not.
When remote care is reasonable
Telehealth often works well when:
-
You have familiar symptoms: Itching, burning, mild bleeding with bowel movements, or recurrent fissure-type pain.
-
You need convenience: Work, childcare, or distance can make office visits hard.
-
You want discreet care: Many people delay treatment because they are embarrassed.
When you need an in-person exam
Some symptoms should push you toward urgent or direct evaluation.
| Symptom | Why it matters |
|---|---|
| Heavy bleeding | The source may not be a simple hemorrhoid |
| Severe swelling with intense pain | Could be a thrombosis, abscess, or another acute issue |
| Fever or drainage | Infection needs prompt assessment |
| Black stools | Bleeding higher in the digestive tract is possible |
| New pain with a mass or major change | The diagnosis should be confirmed in person |
If your symptoms are escalating or do not fit the usual pattern, the safest move is a hands-on exam.
Frequently Asked Questions
How fast does lidocaine hydrocortisone cream work
Patients often notice that the pain relief starts working immediately after application. That makes sense because lidocaine is a numbing medicine designed for quick local relief.
Hydrocortisone works on inflammation, so that part is not always felt as instantly as the numbing effect.
How long does healing usually take
Symptom relief and healing are different. In patient feedback shared in the author brief, healing usually takes about 2 weeks.
That timeline can be shorter or longer depending on the diagnosis, bowel habits, and whether there is ongoing sphincter spasm, constipation, or repeated irritation.
Is lidocaine hydrocortisone cream over the counter
The lidocaine hydrocortisone cream discussed here is typically a prescription product for anorectal use. That matters because anorectal symptoms are easy to mislabel. What seems like a hemorrhoid can sometimes be a fissure, dermatitis, infection, or another problem entirely.
Prescription review helps match the treatment to the condition.
Can I use it if I am pregnant or breastfeeding
Possibly, but this is a situation where your provider should weigh in. Pregnancy and postpartum hemorrhoids are common, yet safety data for this combination is limited, so individual review is the right move.
If you are pregnant, trying to conceive, recently postpartum, or breastfeeding, tell the prescribing provider before using it.
What if I cannot find my prescription locally
Stock issues happen, especially with less common prescriptions and compounded medications. If you are calling around to locate a medication, a practical resource on how to find a pharmacy close to me with medication in stock can make that process less frustrating.
It is also worth asking whether a compounding pharmacy is the better fit for your prescription. Of course, you are always able to access these medications through Bummed .
If you want specialized anorectal care without the usual wait, Bummed offers online evaluation and custom, surgeon-formulated prescription creams for hemorrhoids, fissures, anal itching, and related conditions. Their formulations may combine multiple active ingredients, including lidocaine and hydrocortisone with other evidence-based ingredients, based on your symptoms and clinician review.
Bummed content is for general education and should never replace professional medical advice that considers your individual health. If you think you’re experiencing a medical emergency, call 911 or head to the nearest emergency department.
Prescription products require an online consultation with a physician who will determine if a prescription is appropriate.
